A currently trending social media lingo is “ment or malaria?” and whenever I see or hear it, cerebral malaria easily comes to mind. In essence, the question “ment or malaria?” is posed to someone who asks a seemingly meaningless question or makes an irrelevant comment. So it’s like the person is being asked: “Is your comment driven by mental troubles or malaria?” – referencing the myth that malaria can affect the brain.
But, then, is this really a myth? Can malaria affect the brain? Cerebral malaria, a complication of severe malaria, affects the brain. However, the clinical presentation of cerebral malaria is entirely different from what the lingo suggests.
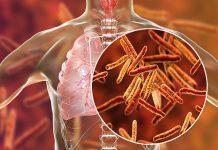
Here is a brief refresher. Malaria is still one of the most prevalent infectious diseases in the world. In fact, according to the World Health Organisation (WHO), there were 241 million malaria cases in 2020 and 627,000 deaths. Of this figure, the African region carried a disproportionately high share of the global malaria burden being home to 95 percent of all malaria cases and 96 percent of deaths, with Nigeria contributing the highest burden. Children under five years accounted for 80 percent of all malaria deaths in this region.
Malaria is a life-threatening disease caused by Plasmodium parasites, spread by infected female Anopheles mosquitoes. The infection clears with appropriate medications. In other cases, however, complications may arise, ranging from renal failure and anaemia to metabolic alteration and cerebral malaria.
Hypoglycaemia
- Hypoglycaemia is a critical complication of malaria in three groups of patients:
- Patients with severe diseases, especially young children
- Pregnant women, whether on admission or after quinine treatment
- Other patients treated with quinine as a result of quinine-induced treatment
Clinical presentation: In conscious patients, it may present as sweating, breathlessness, dilation of pupils, tachycardia, breathlessness, anxiety, a feeling of coldness, and light-headedness. If these continue without clinical intervention, patients may lose consciousness. Hypoglycaemia may also cause generalised concussions and posturing.
Hypoglycaemia is frequently overlooked because its symptoms also present in severe malaria itself. Deterioration in consciousness is also a hallmark feature of hypoglycaemia, but it is also a warning presentation of cerebral malaria.
Cerebral malaria
It is reportedly the most severe neurological complication of P.falciparum infection. It may occur less than two weeks after a mosquito bite and develop after two to seven days of suffering from a fever. The WHO defines cerebral malaria as a clinical syndrome characterised by coma at least one hour after termination of a seizure or correction of hypoglycaemia, with asexual forms of P. falciparum on peripheral blood smears and no other cause to explain the coma. Cerebral malaria is an important complication of malaria in children.
Pathogenesis: Attempts to understand the pathogenesis of cerebral malaria mostly rely on the brain tissues of patients who died from the condition. A histopathological finding is the intense sequestration (or segregation) of infected erythrocytes in cerebral microvessels. An autopsy series of patients who died from cerebral malaria revealed that 94 perfect of their brain microvessels contained adherent infected erythrocytes, compared with 13 percent in patients who died from non-cerebral malaria. It is suggested that cerebral sequestration of infected red blood cells is the aetiology that leads to cerebral malaria.
Symptoms/clinical presentation: A hallmark symptom of cerebral malaria is impaired consciousness, with coma being the most severe clinical manifestation. Coma onset can be gradual or sudden. When cerebral malaria develops gradually, patients initially present with drowsiness (this symptom should be considered worrying), confusion, delirium, or agitation.
Other symptoms include: open-eyed but non-seeing; disconjugate gaze, Nystagmus, sustained ocular deviation, usually upward or lateral, abnormal posturing, seizures and electroencephalographic (EEG) abnormalities, fixed jaw closure, and tooth grinding.
Severe anaemia
Rupture of the red blood cells (haemolytic anaemia) occurs with malaria. However, in the case of severe malaria, dangerously low RBC count or diminished RBC function ensues. Anaemia may be associated with a secondary bacterial infection. It is a significant complication of malaria in pregnant women.
Clinical presentation: fatigue, headaches, low blood pressure.
Acute renal injury
Sometimes, P. falciparum parasites in the RBCs may block tiny vessels in the kidneys; or RBCs may clump due to toxins, interfering with normal kidney function and causing pain.
Malaria in pregnancy
In a malaria-endemic settings, such as Nigeria, pregnant women are highly susceptible to severe anaemia. Severe malaria is associated with higher mortality in pregnancy than in non-pregnant women.
Pregnant women with uncomplicated malaria have increased risks for abortion, stillbirth, premature delivery, and low birth weight. However, severe malaria usually causes premature labour, stillbirth, and death of mother and/or child. Severe malaria may also present immediately after labour where postpartum bacterial infection is a common complication.
Globally, the incidence of severe malaria is on the decline, thanks to better therapy options and greater awareness. However, several cases of cerebral malaria and other complications of malaria come up, especially in developing countries; but the incidence is low.V